Finally free as a bird with one dicked-up wing. “Fly like an eagle…to the sea. Fly like an eagle, let my spirit carry me.” Yeah, right. More like a lyrebird with a bandaged wing. In case you didn’t know, they are very awkward flyers, and thus spend most of their time on the ground. You can read more about them here.
Anyway, on my way home I unfortunately felt every bump, dip, sharp curve, and too-fast braking. However not nearly as awful as it could have been, as my husband happens to be one of the best drivers I’ve ever seen or had the pleasure of riding with. He expertly handled the winding country roads for the last half hour of our trip as gently yet efficiently as he could.
Roads like these always seemed like so much fun to travel on. Truth be told, they absolutely are…just not when you’re in severe pain or nauseous. I still highly recommend taking the “scenic routes” wherever you reside at least once. The experience of driving through beautiful countryside is thrilling, peaceful, and highly enjoyable.
Naturally, the nausea kept coming in waves, though thankfully I did not actually vomit. That would have hurt like a mother effer. The pain on the way home, however, was quite fierce. I found myself wishing they would have sent me home with some one-time use ice packs. I may have to mention that in the patient experience survey.
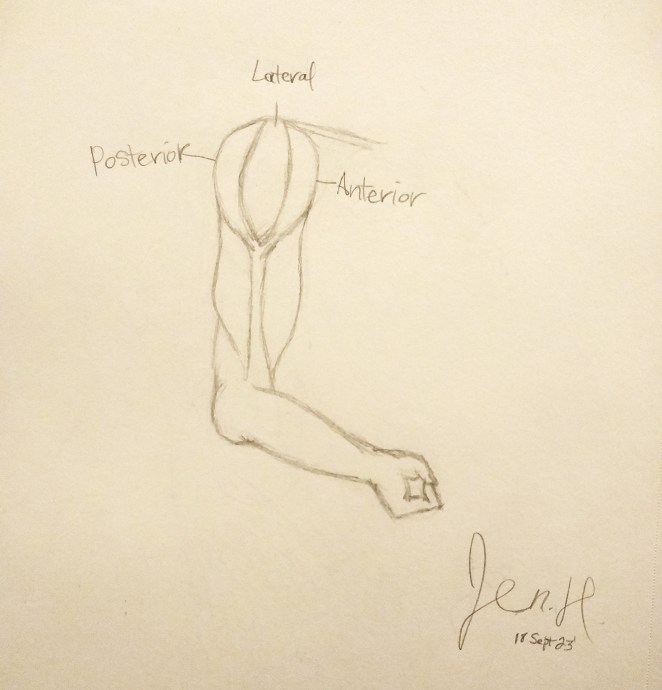
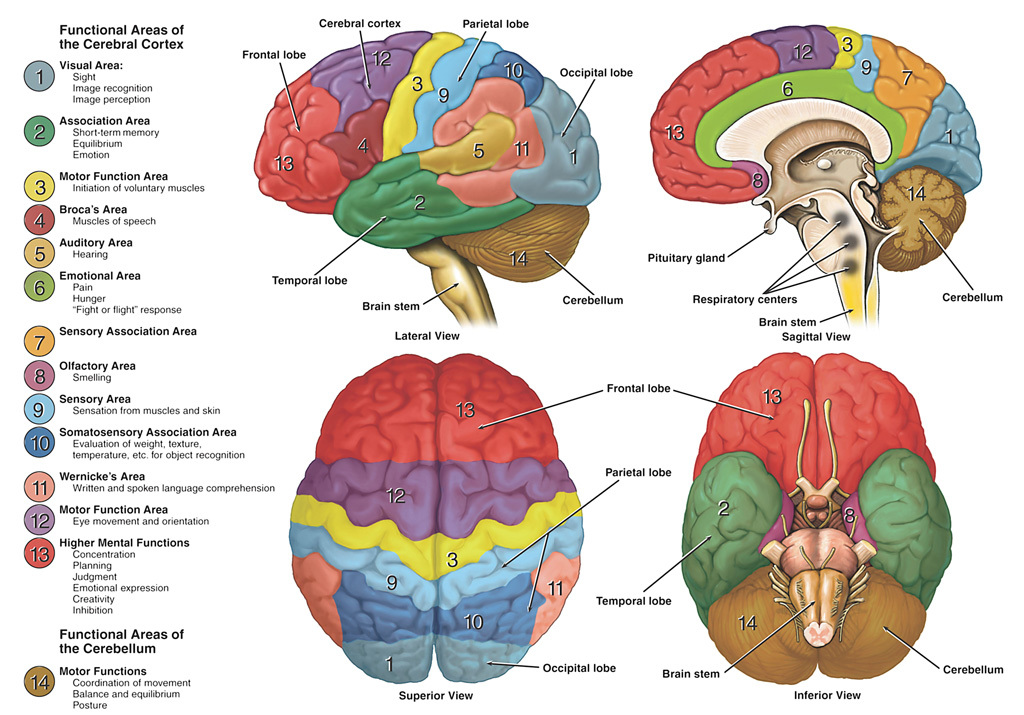
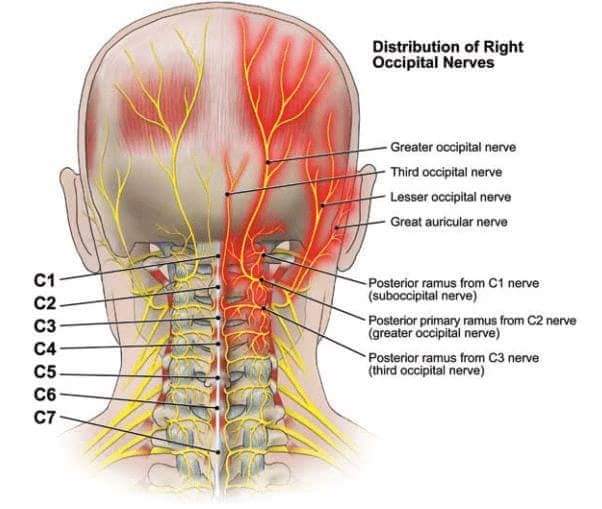
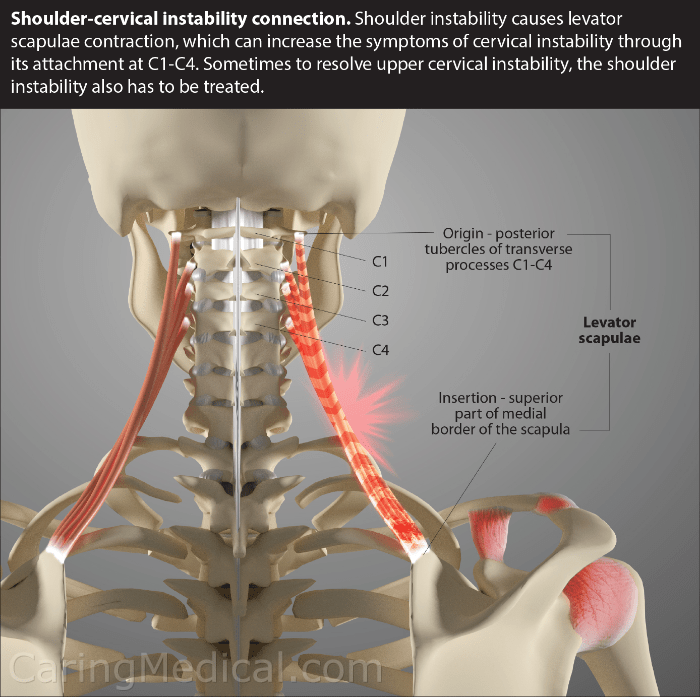
Oddly enough, most of my pain wasn’t at the incision site. Neither was it located at the target area where he worked his magic to mend the musculature in my shoulder blade. Instead, it manifested in the shoulder joint, predominately on the anterior and lateral sides (see above diagram). In those spots, it felt like somebody took a hammer to it, and left a big screwdriver in there.
The rest of the day was difficult, with drifting in and out of sleep, keeping the nausea at bay, and controlling the pain as best as I could. The pain meds, muscle relaxers, and ice packs were my best friends, and the only way I slept at all that night. The nighttime was equally unyielding, sleeping only one to two hours at a time on average.
DAY 2 of RECOVERY:
By morning, however, the dark clouds of agony had cleared a little. I felt stiff and sore, despite moving my elbow joint and flexing my hand periodically as I was supposed to. At any rate, I was still significantly better off than I was the day before.
To my pleasant surprise, both a recovery nurse and Dr. Grantham’s Physician Assistant called to check on me today, as well as to provide me further instructions for the days to follow. Even in the throes of the worst of the pain, I still feel that this was the right decision, and I’m glad that I did it. I know it will all be worth it in the end.
If you can’t tell, those pain meds are working wonders right now.
DAY 5 of RECOVERY:
I finally got to take a shower today, YAY! It was challenging and awkward, but I managed. Between a washcloth, a loofah, and a shower chair, mission accomplished. It’s worth mentioning that the shampoo and conditioner bars I switched to a few months ago made washing my hair one-handed remarkably easier than using standard liquid shampoo. Unexpectedly, toweling off afterwards proved more challenging than showering.
It is definitely a strange feeling being stuck at ninety degrees (and lower) range of motion with that arm…somewhere between having a robot arm and a ragdoll arm. Besides that, the whole area is still achy and sore, although much more tolerable than the first few days. I’ve graduated to managing the pain with only NSAIDs, muscle relaxers, and ice at the moment. I’m thankful for that, because I am not a fan of the side effects.
Not to mention the pain in the neck it is to get narcotic pain medications at all (yes even for surgery), much less a refill, thanks to the knee-jerk policies of our government. Meeting at a commonsense middle-ground between sustaining patient care and avoidance of bolstering opioid addiction numbers never quite seems to be within their grasp.

It’s like, “Excuse me, I don’t want to take this crap in the first place, but I’m having surgery, and would rather not be in extreme pain waiting for it to be filled. Yes, I am well aware I have not had the surgery yet, but I prefer a proactive approach, rather than having to send my caretaker back out for it when I need them by my side. By handling it myself beforehand, I save us both a great deal of hassle.”
I find having to explain all of that and justify why I need them at all, particularly beforehand, absurd. That is what my doctor is there for, a practicing surgeon. If that doesn’t clue the powers that be in for the need, feel free to call the clinic, who will then tell you that yes, I am indeed scheduled for surgery, and will be in a f*#kload of pain when I wake up. Painstaking as the process of getting these medications filled may be, I know it’s not the pharmacy’s fault. They didn’t make the rules, they are just forced to follow them.
DAY 6 of RECOVERY: WORST NIGHT OF SLEEP SO FAR…
As was the routine, I felt snuggled up with all the pillows and soft warm blankets, all settled in when I shut off the light, eyes and mind too tired to keep reading. Or so I thought. Then the restless legs began. If you have never experienced that sensation, it’s like a reflex test at the doctor, but in your calves, and constant.
The urge to move your legs is irresistible and involuntary, a feeling like you need to kick something or sprint across the yard. It’s hard to explain but very uncomfortable and definitely not something you want to experience when exhausted and trying to sleep.
At this point, I thought of my friend Brittany, who has early onset Parkinson’s disease. She once described a similar sensation of not being able to stop her legs from involuntarily moving caused by dystonia related to her Parkinson’s. My heart filled with sympathy for her all over again.
With the aid of my handy walking stick, I have been walking daily. Short bursts in the house at first. It’s a healthy distraction from the pain and helps with the boredom. Apparently, experts agree that walking also aids in recovery and helps prevent post-surgical complications such as blood clots.
By day 3 or 4, I was walking outside, increasing the time and distance each day. It was quite tiring in the beginning, but this light exercise definitely sped up my recovery and gave me a much-needed mental health boost. I began looking forward to my daily walks embracing the birdsongs, studying mushrooms I found, the smells and scenery of the forest. I suppose that is one of the best things about living in the middle of nowhere, Kentucky.

So, I knew the restless legs weren’t occurring due to lack of physical activity. I also ruled out any of the medications I was taking as the root cause. I drink caffeine in moderation, only one mug each morning upon waking. So what gives?
My theory is that my body declared, “I’m not sleeping in that damn chair anymore. And um, hello, did you forget you are not a back sleeper?!” and I was like, “Well ok, but couldn’t you have said something earlier in the evening? Possibly before my husband (and caretaker) went to bed himself, perhaps? Now what the flip are we going to do???”
I tried walking, stretching, massaging, and exercising my restless legs with calf raises. That combination seemed to help so I crawled back in the chair, piled my blankets back on, and tried once again to sleep. Next came the back pain. The muscles in my back suddenly spasmed and the ache was particularly intense around my kidneys and middle back. It’s similar to the cramping that can occur in that area as a result of sleeping for too long of a stretch.
“Not being able to sleep is terrible. You have the misery of having partied all night… without the satisfaction.”
-Lynn Johnston, Canadian Cartoonist
It’s as if your body says, “We’ve slept quite enough, thank you. Here’s some back pain to motivate you to get the hell out of bed, NOW.” Except I hadn’t had any sleep. I wrestled about (gently) for an hour or two more, at which point I felt the urge to get up again. Let’s try the couch, I thought.
Seemed like an easy way to test out if I was ready for side sleeping on the uninjured arm. I didn’t want to be bothering the hubs or moving all 6 pillows, water, and eye mask to the bedroom one-handed, in the dark, without knowing for certain.
Thus, I placed a pillow under my injured arm, one under my head, and threw on a warm sherpa throw blanket (yes it is as lovely as it sounds, you should totes muh-goats get one). Almost instantly after getting situated for my experiment, I passed out into a halfway sleep. A far sight better than previous attempts, I considered this a success.
Around 5 a.m. my husband awoke, and after giving him a brief synopsis of my sleep struggles, I awkwardly climbed into bed. He helped me with the covers, and I was out like a light bulb. I slept a deep, dreamless sleep for about 3 hours.
While 3 hours is certainly not much and a far cry from the recommended 7-9 hours, I felt grateful for those few precious hours over none at all. Besides, I thought, I can always squeeze in a nap today if needed. My only focus right now is healing and listening to my body (and my surgeon’s instructions).
This includes resting when I need to, whether I want to or not. I find that at this point, even when I do achieve a decent night’s sleep, I still need an afternoon siesta. Many times, I conk out hard enough during these naps to reach REM, resulting in some weird, eccentric dreams. That may be partly due to the meditation channel (see below) I’ve been plugging into during those naps, in hopes of preventing my family’s daily noises from disturbing my rest.
I guess I wasn’t expecting this part to be so challenging. I wasn’t prepared for my body to reject the position or location of sleep so early on. Maybe this is a good sign that I am healing well and swiftly. It sucks that I must be in this sling for 36 more days. Yes, I am counting down the days. I have found this to be helpful many a time when traversing something difficult, going through a hard time, or just feeling stuck in life.
Whether that calls for breaking up a tough time into measurable chunks with things to look forward to, or breaking up a long-term goal into smaller ones…I find it is always helpful. In example, the journey to get this shoulder surgery took 3 years of concentrated effort. Being that it was not the only medical puzzle I was trying to solve during those three years, it was hard. But mapping a path forward for reference, made it more bearable.
However, in the throes of recovery, it is also important to celebrate even small wins. For example, I figured out how to button my husband’s jacket over my sling one-handed today! It doesn’t seem like much, but it is a small victory to me. While I understand the necessity of asking for help sometimes, I relish being able to do things for myself.
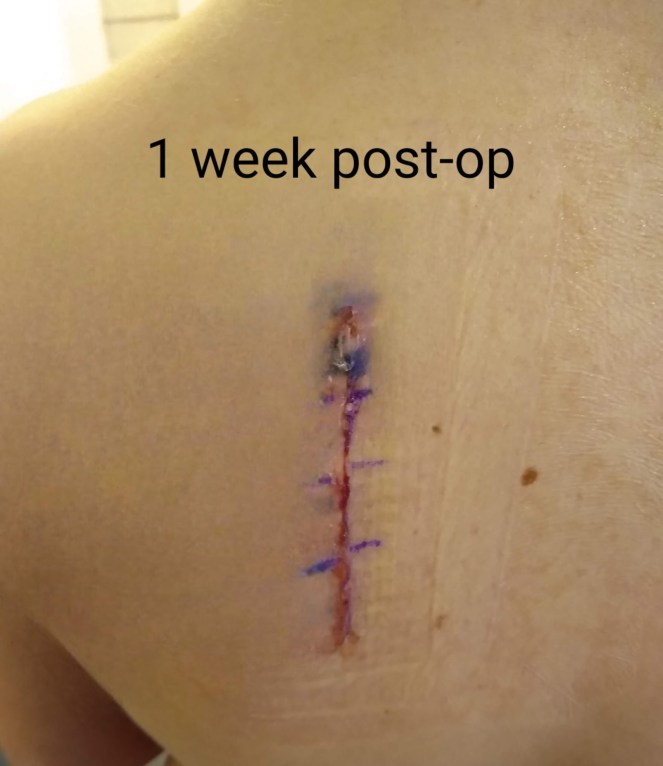
For another small win, I am nearly entirely free of needing pain medication, including the muscle relaxers and ibuprofen. My doctor may still want me on anti-inflammatories for healing purposes, but I’m celebrating hardly needing them for pain anymore! I do not like taking pills. Better still, I have finally made it through the first week of recovery! Here’s a look at how I am healing!